What is a Peripherally Inserted Central Catheter (PICC)?
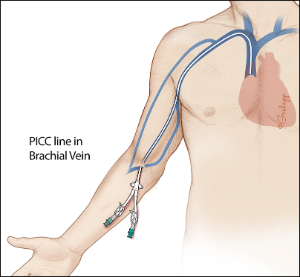
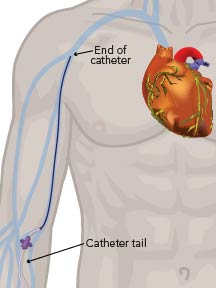
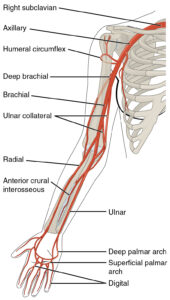
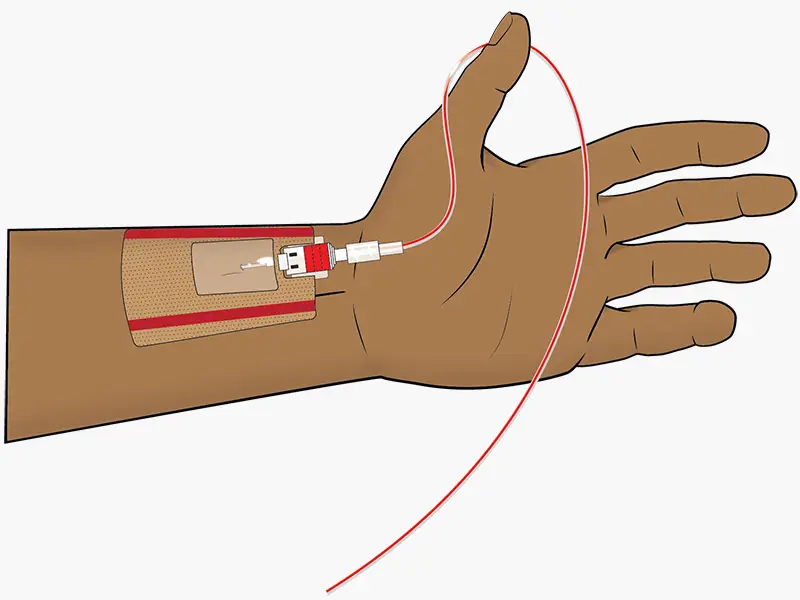
A peripherally inserted central catheter (PICC) is a long, thin tube that goes into your body through a vein in your upper arm. The end of this catheter goes into a large vein above your heart called the Superior Vena Cava (SVC).
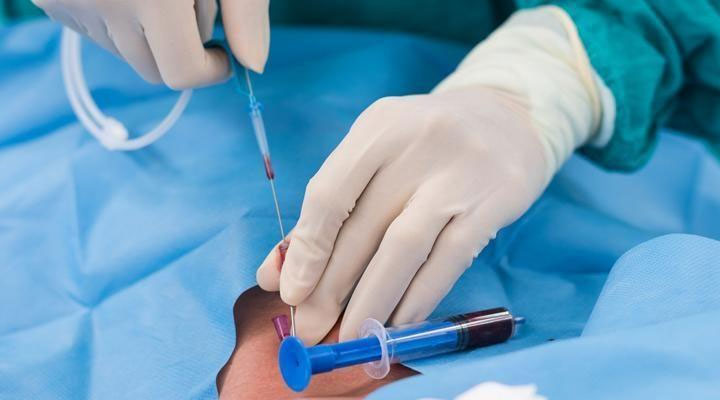
- The PICC is used to carry nutrients and medicines into your body. It is also used to draw blood when you need to have blood tests.
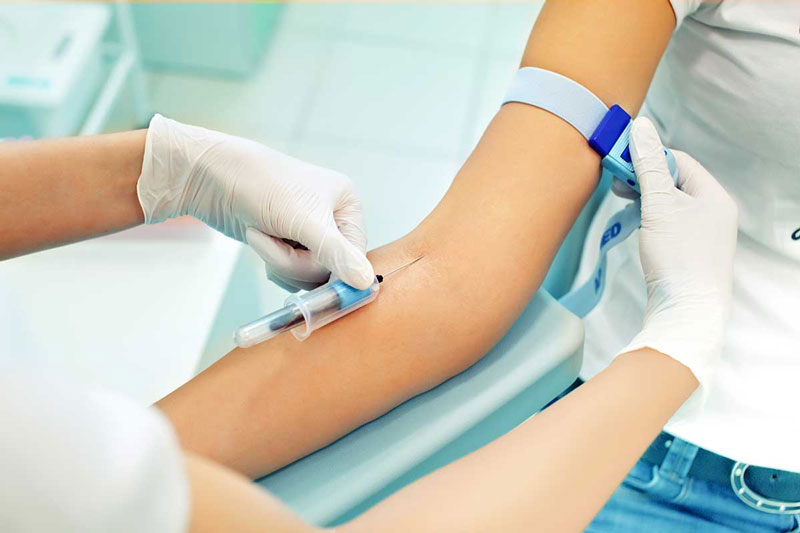
- A PICC is used when you need intravenous (IV) treatment over a long period of time or if blood draws done via venipuncture have become difficult.
- A PICC can also be used for Chemotherapy drugs.
Our staff has the ability to perform these types of lines in the Home, Clinic, and Hospitals. We use Ultrasound and 3CG Technology helping clinicians have the highest success rates in the industry.